The Cell That Builds Your Face
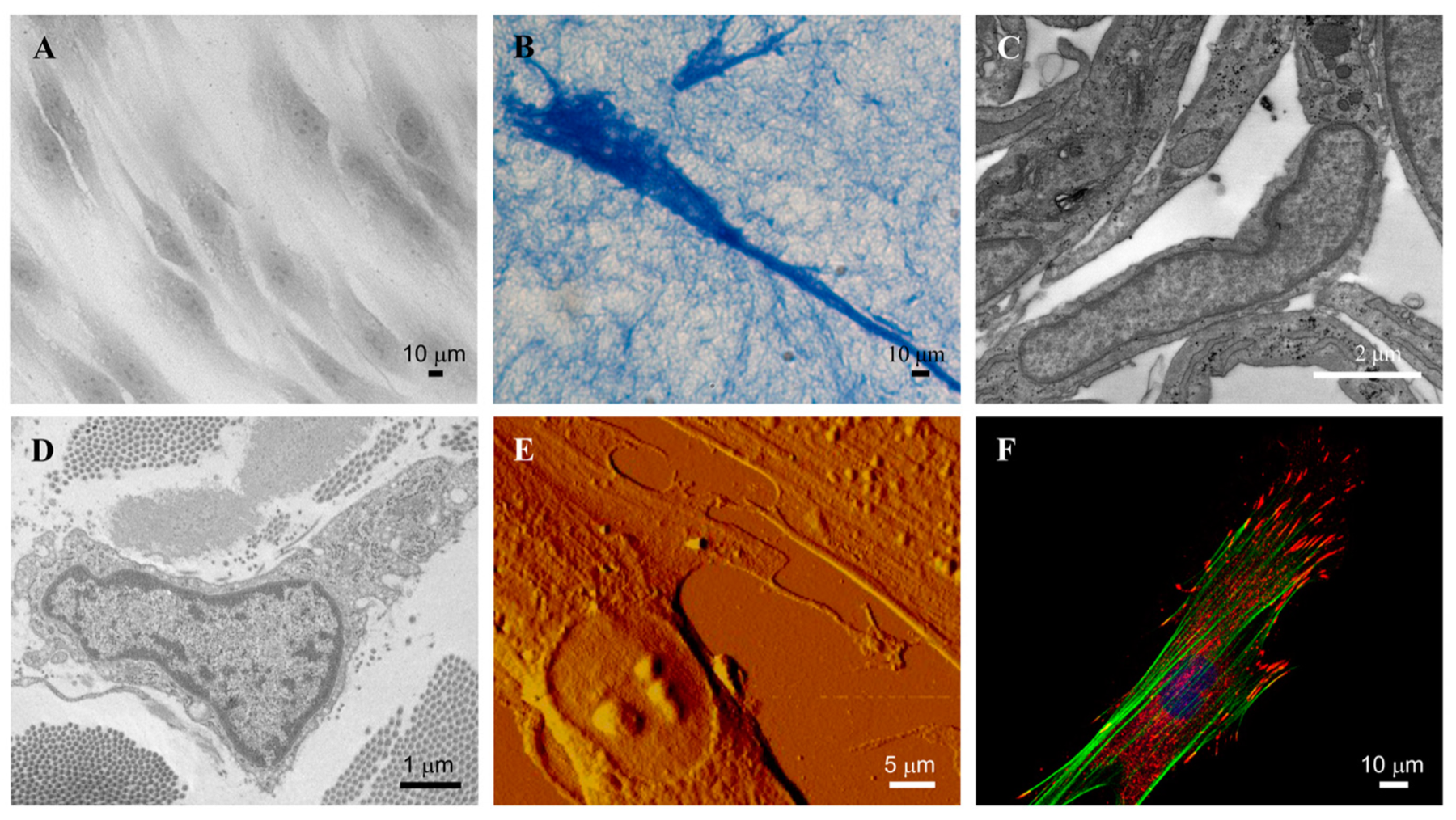
If you want to understand why skin ages, you must understand the fibroblast. This spindle-shaped mesenchymal cell, resident in the dermis, is the primary manufacturer of the extracellular matrix — the biological scaffold of collagen, elastin, and glycosaminoglycans that gives your skin its structure, resilience, and volume. When fibroblasts are metabolically active and well-stimulated, your skin reflects it. When they are senescent, mechanically uncoupled from their matrix, or operating in a pro-inflammatory microenvironment, that story is written visibly on the skin surface as well.
The fibroblast does not merely produce collagen and wait. It is a dynamic cell that continuously senses mechanical signals from the ECM, responds to growth factor gradients, integrates hormonal cues, and modulates its output accordingly.
The Molecular Pathway: From Gene to Fibril
Collagen synthesis is a multi-step intracellular and extracellular process. It begins in the nucleus, where the genes COL1A1 and COL1A2 are transcribed in response to regulatory inputs including TGF-β/Smad signaling, mechanical tension via integrin-focal adhesion complexes, and retinoid receptor activation.
This assembly is critically dependent on the post-translational hydroxylation of proline and lysine residues, a biochemical reaction catalyzed by prolyl 4-hydroxylase and lysyl hydroxylase, both of which require L-ascorbic acid (vitamin C) as an essential cofactor. The triple helix cannot form without an adequate number of 4-hydroxyproline residues.
The clinical implication for aesthetic medicine is precise: vitamin C is not an optional supplement for skin health. It is a rate-limiting biochemical requirement for every collagen molecule your fibroblasts produce.
The Mechanosensing Problem: Why Aged Fibroblasts Stop Building
A critical and underappreciated dimension of fibroblast biology is mechanotransduction — the process by which cells sense and respond to the mechanical properties of their surrounding matrix. Fibroblasts require physical tension from the collagen matrix to maintain active synthetic function.
When matrix tension is adequate, integrins activate FAK (focal adhesion kinase) and downstream Rho/ROCK signaling, sustaining fibroblast spread morphology and maintaining procollagen synthesis. When this feedback loop breaks down in aging skin, as MMPs fragment collagen fibrils, the mechanical tension is lost.
Senescent Fibroblasts: Active Destroyers, Not Passive Failures
Senescence is not simply cell death or dormancy. It is a distinct, stable cell state characterized by irreversible cell cycle arrest, dramatic metabolic reprogramming, and the acquisition of the Senescence-Associated Secretory Phenotype (SASP).
Senescent fibroblasts express MMP-1, MMP-2, MMP-3, and MMP-9 at levels significantly elevated above non-senescent controls, while simultaneously downregulating COL1A1 and COL3A1 mRNA. The SASP components — including IL-6, IL-8, and TNF-α — create a chronic low-grade inflammatory environment that induces senescence in neighboring fibroblasts through paracrine signaling.
Four Clinical Levers: What the Evidence Supports
Understanding the biology of fibroblast decline allows us to map the mechanisms of effective interventions with precision. Four modalities have robust evidence for fibroblast stimulation:
Topical retinoids upregulate COL1A1 and COL3A1 transcription, increase TIMP expression to suppress MMP-mediated degradation, and activate AP-1 suppression pathways. A 2025 review confirmed wrinkle reduction of 40–60% at 6–12 months with tretinoin 0.025–0.1%.
Microneedling activates fibroblasts through controlled mechanical injury. TGF-β-1 and -2 are upregulated within 24 hours, and TGF-β-3, the anti-fibrogenic isoform that promotes organized collagen lattice, remains elevated past eight weeks.
Radiofrequency recruits fibroblasts through controlled thermal injury, with histological studies documenting significant increases in collagen and elastic fiber density.
PLLA biostimulants activate fibroblasts through the foreign body response pathway via TGF-β/Smad signaling, sustained over months as particles degrade slowly.
The Layered Protocol: Why Mechanism Diversity Is the Point
None of these interventions is a complete solution in isolation. Each addresses a different upstream node in the fibroblast biology network. Tretinoin optimizes the baseline transcriptional environment. Microneedling creates a wound-healing window with enhanced absorption. RF provides deep volumetric heating that reaches fibroblast populations that surface-level interventions cannot access. PLLA provides a sustained months-long depot signal.
Together, they address the fibroblast economy from the supply side (synthesis stimulus), the demand side (degradation suppression), and the structural side (matrix tension restoration).
The fibroblast is not passive. Neither should your treatment plan be.